Have you noticed that some of our actions or behaviors are not carried out consciously? The truth is that we are not fully aware of everything that happens inside our brain like all the connections triggered when an emotion or thought suddenly appears in our mind. Instead, we know that the major brain activity is highly driven by both, internal biological signals linked to the autonomous system and external cues coming from the environment. Apparently, all these brain activity generators are beyond our conscious control. But is this really the case?

A key to direct our cognitive performance
Generally speaking, cognitive performance is defined as the optimal execution of activities that involve multiple mental abilities (e.g., Pattyn et al. 2008; Roy, 2013). From a cognitive psychology perspective, cognitive performance entails managing various interacting processes such as perception, alertness, attention, memory, or executive functions like working memory. Such a number of brain processes are often assessed indirectly, through neurocognitive tools like measurements of response times or accuracy levels in the context of task performance.
Psychological and physiological factors such as fatigue, stress, motivation (Newell et al. 2008; Sutarto et al. 2010), and mood imbalances (Sutarto et al. 2013) can have a huge influence on cognitive functioning. Sometimes these factors can prevent someone from performing optimally in normal life activities, negatively impacting daily performance.
What if we can have control over those hinder factors by simply learning how to track and train the activity of our neurons?
The main goal of Neurofeedback (NFB) therapy is to modulate the brain’s (dys) functions by regulating emotions and directing the attention focus. By improving the brain’s ability to shift between arousal states of excitement and relaxation, the related neural pathways can be either over-activated, under-activated, or dysregulated accordingly. Such neural adjustments result in an overall enhancement of mental performance, emotional management, and mood stability (Sitaram et al., 2017).
Neural mechanisms of brain (dys) functions
From scientific studies, we know that our brains contain billions of neurons that fire and communicate at the same time. There is an old saying in neuroscience that “neurons that fire together wire together”. This basically means that the more a neural-circuit runs the stronger that circuit becomes.
In the context of NFB therapy, understanding the specific brain mechanisms underlying cognition is key to directly alter defective neural pathways causing dysfunctional behavior (Başar et al., 2016; Enriquez-Geppert et al., 2017). For example, we know that anxiety disorders are characterized by an excess of activity in the parietal and occipital lobes. The treatment hence is focused on reducing or deactivating neural pathways involved.
Thanks to advances in brain technology it is possible to identify specific neural circuits that are relevant to emotion, motivation, and cognition functioning. When those neurons communicate with each other, they produce synchronized electrical impulses that result in brainwaves. To understand the fundamentals of neurofeedback, we must first understand how brainwaves work.
Fig.1 Learning how to control or cognitive performance with neurofeedback involves the modulation of neural pathways underlying (dys) functional brain activity
Learning more about Neurofeedback: brainwaves
Any behavior, emotion, or thought has associated a stream of brainwaves that can be differentiated based on its oscillatory frequency (measured in cycles/seconds or Hertz). Depending on the particular brain state or activity, the waves alternate between the following rhythms:
- Delta brainwaves (1 to 4 Hz): This pattern occurs during deep stages of sleep when restorative processing is taking place. Having too little of this brainwave indicates a pattern of poor sleep, insomnia, or dissociation (Knyazev, 2012). Pathological delta activity is observed in awake states consistent with generalized encephalopathy and focal cerebral dysfunction (Nayak et al., 2020).
- Theta brainwaves (4 to 8 Hz): The brain is in this frequency band when we are in deep relaxation, and our mind wanders off or it is immersed in deep meditation. Excessive theta correlates with fatigue, hypnotic states, like the one experienced during highway hypnosis or freeway driving (sensation of falling sleep with eyes open; Craig et al., 2012).
- Alpha brainwaves (8 to 12 Hz): Mostly predominates during a mindful state of calmness, sense of ease and relaxation, such as when a person is resting down after completing a task. It represents a non-aroused state of mind (Mireau et al., 2017; Zhang et al., 2012). Atypical alpha activity, especially in frontal areas, is often associated with adult ADHD and depression (Jaworska et al., 2012; 2012). An imbalance in alpha wave activity is consistent with alertness, agitation, irritability or avoidance behavior among other severe pathologies like substance addiction (Meda et al., 2019; Tayama et al., 2017).
- Sensorimotor rhythm (SMR) brainwaves (12 to 15 Hz): This wave pattern is associated with an attentive state of mind like when one is alert navigating in virtual reality but without any movement (Scherer et al., 2008; Timmers, 2014). Imbalances in such activity can drive you to a depressed mind state or inattentiveness.
- Beta brainwaves (15 to 32 Hz): These waves represent the fastest processing speed that typically occurs when the brain is externally focused, actively engaged in critical reasoning, thought, or highly concentrated performing an activity. When awake, most people exhibit beta wave patterns. Excessive beta activity is a marker of a stressful mind, rumination likely indicating emotional distress (Hamid et al., 2015; Hayashi et al.,2009 )

Through the use of non-invasive brain-computer technology (EEG recordings), Neurofeedback therapy monitors brainwaves activity and trains the patient to self-regulate itself. This simply means to become aware of your own brain functioning processes allowing you to think and function at a more efficient level.
In a way, NFB training could be compared to having a teacher by your side kindly pointing out your errors and then, helping you in knowing when and how to correct them.
Interesting but…how it works?
With Neurofeedback, an individual presenting a certain cognitive, behavioral, or affective deficit (e.g. attention deficit disorder, addiction disease, anxiety), can learn to adjust his/her EEG activity to mirror the desired pattern of cortical activity, and thus, perform better in daily basis. Such changes in the EEG pattern results in changes in the targeted behaviors. The way to manage this is by means of a rewarding visual and/or auditory feedback process.
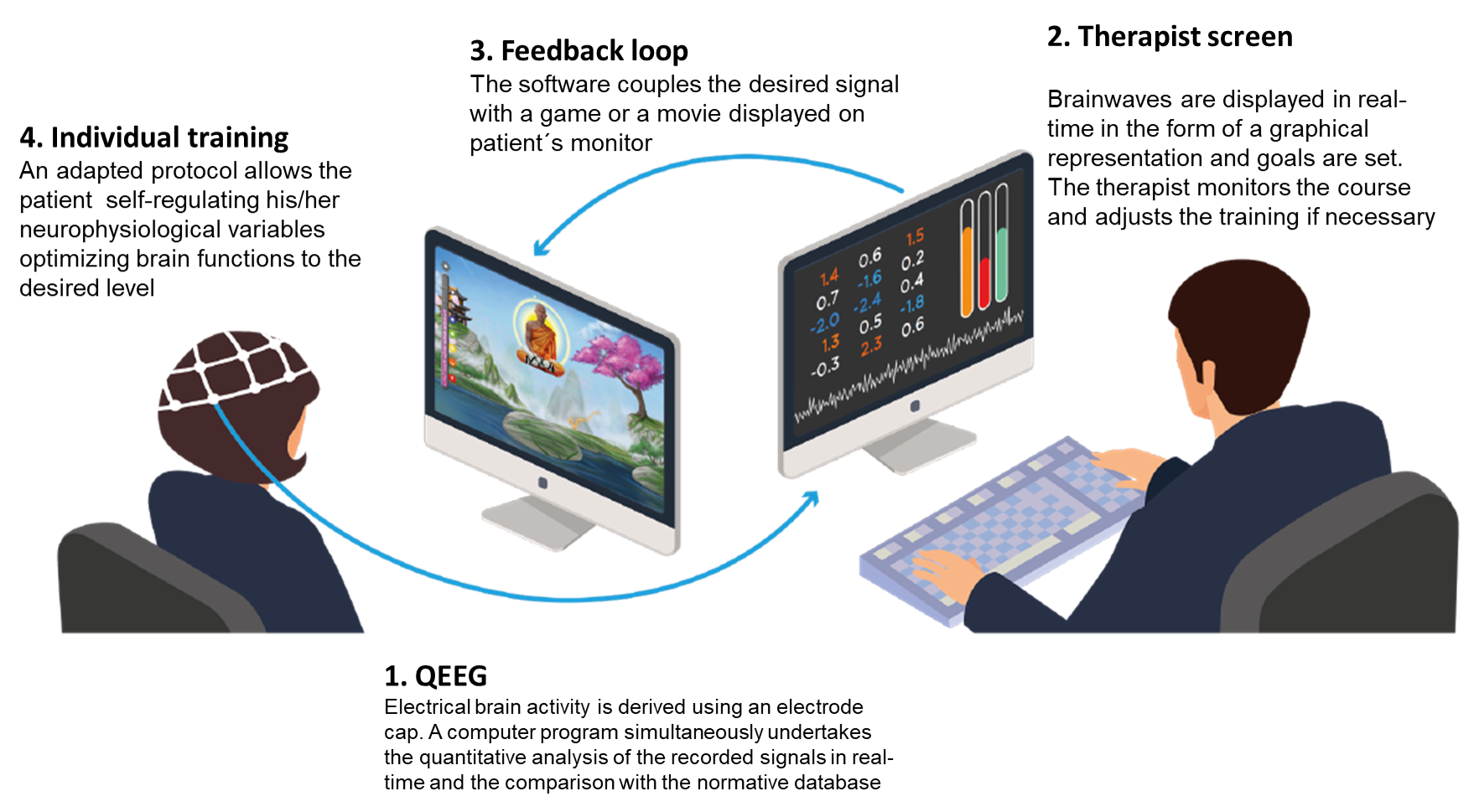
A neurofeedback session begins with an EEG recording sequence that is completely directed or piloted by computer-based protocol, allowing monitoring brainwaves in real-time. Meanwhile, the system provides feedback to the user during the experience of the rewarding activity. Each time the desired EEG pattern occurs, the program maintains “on” the rewarding activity (e.g. music, video game, or movie). Instead, every time undesired EEG signals appear, the program stops the rewarding activity.
If you think carefully, what is really going on is just an operant (or instrumental) conditioning learning process. Indeed, part of the success of neurofeedback in brain self-regulation relies on such a basic learning mechanism (Dessy et al., 2018). But the true “main character” in all this equation that explains why it definitely works so well, has to do with an amazing brain property called neuroplasticity.
Neurofeedback and brain plasticity: how do they relate?
Neuroplasticity is defined as the brain’s ability to alter its organization and connectivity patterns, based on new learning experiences and behaviors (Berlucchi and Buchtel, 2009)
The NFB therapy takes advantage of neuroplasticity to re-wire the brain allowing achieving a particular cognitive improvement, or even enabling more global treatment of several psychological/psychiatric disorders. With sustained training during a sufficient period of time, the patient will gradually reorganize his neural connections optimizing brain functioning.
A common question is whether the achieved changes last long-term after receiving enough training. When modifications in the brain have been physically (changes in neuron morphology) and functionally accommodated (neural connectivity), they end up being automated, and therefore, they last almost for entire life (Shaffer, 2016).
Who can benefit from Neurofeedback?
The proven benefits of Neurofeedback have been found to be beneficial in treating a variety of cognitive and affective disorders including attention-deficit/hyperactivity disorder (ADHD), depression, anxiety, post-traumatic stress disorder (PTSD), autism, and epilepsy among others. Also, it has been shown to be highly effective in the rehabilitation of traumatic brain injuries. The main advantage for patients is a progressive optimization of mental health mostly in medical resistant cases.
A variety of EEG-NFB scientifically proven protocols to treat patients are commonly used with excellent results. The so-called alpha augments, alpha/theta training, beta augments, sensorimotor rhythm (SMR) are the ones showing scientifically proven positive results in treating different pathologies (Cheon et al., 2015; . However, these protocols are not generic and in clinical practice, they should be individualized according to the diagnosis and anamnesis of the patient.

Fortunately, healthy people can also benefit from the positive effects of Neurofeedback. In the field of cognitive skills enhancement, it can be very beneficial for elite athletes, artists, or simply for anyone who wants to improve attention/concentration, memory, or creativity (Ring et al., 2014).
Conclusions
Neurofeedback therapy is a non-invasive safe procedure with strong scientific support in the treatment of many problems and disorders. But it has its own pros and cons. To date, many studies have proven its effectiveness over placebo and other pharmacological treatments like in the case of children diagnosed with ADHD (Van Doren et al., 2018). However, the demonstration of more robust clinical effects remains a major handicap in neurofeedback research (Sitaram et al., 2017). In this regard, evidence of sustained or long-term effects of NFB across pathologies needs further investigation in order to determine its validity as a potential pharmaco-replacement therapy (Rogala et al.,2016).
Moreover, the question of how many sessions are needed before a person can achieve the expected changes remains unclear given the high inter-individual variability. Certainly, desired improvements are very much linked to the level of commitment of the person/patient.
What does seem clear whatsoever, is that NFB provides new ways to understand brain-behavior relationships. Thanks to the current horizon in neurotechnological development and contributions of Cognitive Neuroscience research, the acceleration of NFB optimization even further becomes possible within this century.
References
Başar E. Brain oscillations in neuropsychiatric disease. Dialogues Clin Neurosci. 2013;15(3):291-300. PMCID: PMC3811101
Başar E., Güntekin B. (2008). A review of brain oscillations in cognitive disorders and the role of neurotransmitters. Brain Res. 1235, 172–193. 10.1016/j.brainres.2008.06.103
Başar E, Gölbaşı BT, Tülay E, Aydın S, Başar-Eroğlu C. Best method for analysis of brain oscillations in healthy subjects and neuropsychiatric diseases. Int J Psychophysiol. 2016;103:22-42. doi:10.1016/j.ijpsycho.2015.02.017
Berlucchi, G., Buchtel, H.A. Neuronal plasticity: historical roots and evolution of meaning. Exp Brain Res 192, 307–319 (2009). https://doi.org/10.1007/s00221-008-1611-6
Cheon, E., Koo, B., Seo, W. et al. Effects of Neurofeedback on Adult Patients with Psychiatric Disorders in a Naturalistic Setting. Appl Psychophysiol Biofeedback 40, 17–24 (2015). https://doi.org/10.1007/s10484-015-9269-x
Craig, A., Tran, Y., Wijesuriya, N., & Nguyen, H.T. (2012). Regional brain wave activity changes associated with fatigue. Psychophysiology, 49 4, 574-82 . https://doi.org/10.1111/j.1469-8986.2011.01329.x
Dessy, E., Van Puyvelde, M., Mairesse, O. et al. Cognitive Performance Enhancement: Do Biofeedback and Neurofeedback Work?. J Cogn Enhanc 2, 12–42 (2018). https://doi.org/10.1007/s41465-017-0039-y
(2007) EEG Neurofeedback: A Brief Overview and an Example of Peak Alpha Frequency Training for Cognitive Enhancement in the Elderly, The Clinical Neuropsychologist, 21:1, 110-129, DOI: 10.1080/13854040600744839
Enriquez-Geppert, S., Huster, R. J., & Herrmann, C. S. (2017). EEG-Neurofeedback as a Tool to Modulate Cognition and Behavior: A Review Tutorial. Frontiers in human neuroscience, 11, 51. https://doi.org/10.3389/fnhum.2017.00051
(2012) EEG-Based Personalized Medicine in ADHD: Individual Alpha Peak Frequency as an Endophenotype Associated with Nonresponse, Journal of Neurotherapy, 16:2, 123-141, DOI: 10.1080/10874208.2012.677664
Meda SA, Narayanan B, Chorlian D, et al. Multivariate Analyses Reveal Biological Components Related to Neuronal Signaling and Immunity Mediating Electroencephalograms Abnormalities in Alcohol-Dependent Individuals from the Collaborative Study on the Genetics of Alcoholism Cohort. Alcohol Clin Exp Res. 2019;43(7):1462-1477. doi:10.1111/acer.14063
Mierau A, Klimesch W, Lefebvre J. State-dependent alpha peak frequency shifts: Experimental evidence, potential mechanisms and functional implications. Neuroscience. 2017 Sep;360:146-154. DOI: 10.1016/j.neuroscience.2017.07.037.
Nayak CS, Anilkumar AC. EEG Normal Waveforms. [Updated 2020 Mar 8]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK539805/
N. H. A. Hamid, N. Sulaiman, Z. H. Murat and M. N. Taib, “Brainwaves stress pattern based on perceived stress scale test,” 2015 IEEE 6th Control and System Graduate Research Colloquium (ICSGRC), Shah Alam, 2015, pp. 135-140, doi: 10.1109/ICSGRC.2015.7412480.
Newell, A., Carmichael, A., Gregor, P., Alm, N., & Waller, A. (2008). Information technology for cognitive support. In J. Jacko & A. Sears (Eds.), The human-computer interaction handbook: fundamentals, evolving technologies, and emerging applications (2nd ed., pp. 811–828). Mahawa: Laurence Erlbaum Associates. https://doi.org/10.1201/9781410615862
Newson JJ, Thiagarajan TC (2018) EEG frequency bands in psychiatric disorders: a review of resting-state studies. Front Hum Neurosci 12:521. https://doi.org/10.3389/fnhum.2018.00521
Pattyn, N., Neyt, X., Henderickx, D., & Soetens, E. (2008). Psychophysiological investigation of vigilance decrement: boredom or cognitive fatigue? Physiology & Behavior, 93(1), 369–378.
Ring, C., Cooke, A., Kavussanu, M., McIntyre, D., and Masters, R. (2015). Investigating the efficacy of neurofeedback training for expediting expertise and excellence in sport. Psychol. Sport Exerc. 16, 118–127. doi: 10.1016/j.psychsport.2014.08.005
Rogala, J., Jurewicz, K., Paluch, K., Kublik, E., Cetnarski, R., and Wróbel, A. (2016). The Do’s and Don’ts of neurofeedback training: a review of the controlled studies using healthy adults. Front. Hum. Neurosci. 10:301. doi: 10.3389/fnhum.2016.00301
Roy E. (2013) Cognitive Function. In: Gellman M.D., Turner J.R. (eds) Encyclopedia of Behavioral Medicine. Springer, New York, NY. https://doi.org/10.1007/978-1-4419-1005-9
Shaffer J. (2016). Neuroplasticity and Clinical Practice: Building Brain Power for Health. Frontiers in psychology, 7, 1118. https://doi.org/10.3389/fpsyg.2016.01118
R. Scherer, F. Lee, A. Schlogl, R. Leeb, H. Bischof and G. Pfurtscheller, “Toward Self-Paced Brain–Computer Communication: Navigation Through Virtual Worlds,” in IEEE Transactions on Biomedical Engineering, vol. 55, no. 2, pp. 675-682, Feb. 2008, doi: 10.1109/TBME.2007.903709.
Sitaram, R., Ros, T., Stoeckel, L. et al. Closed-loop brain training: the science of neurofeedback. Nat Rev Neurosci 18, 86–100 (2017). https://doi.org/10.1038/nrn.2016.164
Sutarto, A., Abdul Wahab, M., & Mat Zin, N. (2010). Heart rate variability (HRV) biofeedback: a new training approach for operator’s performance enhancement. Journal of Industrial Engineering and Management, 3(1), 176–198. https://doi.org/10.3926/jiem. 2010.v.
Sutarto, A., Wahab, M., & Zin, N. (2013). Effect of biofeedback training on operator’s cognitive performance. Work (Reading, Mass), 44, 231–243. http://dx.doi.org/10.3233/WOR-121499
Tayama J, Sagami Y, Shimada Y, Hongo M, Fukudo S. Effect of alpha-helical CRH on quantitative electroencephalogram in patients with irritable bowel syndrome. Neurogastroenterol Motil. 2007;19(6):471-483. doi:10.1111/j.1365-2982.2007.00903.x
Takuto Hayashi, Eika Okamoto, Haruhiko Nishimura, Yuko Mizuno-Matsumoto, Ryouhei Ishii & Satoshi Ukai (2009) Beta Activities in EEG Associated with Emotional Stress, International Journal of Intelligent Computing in Medical Sciences & Image Processing, 3:1, 57-68, DOI: 10.1080/1931308X.2009.10644171
Timmers D (2014) Treating attention deficits and impulse control. In: Cantor DS, Evans JR (Hrsg) Clinical neurotherapy. Academic Press, Boston, S 139–169
Van Doren, J., Arns, M., Heinrich, H., Vollebregt, M. A., Strehl, U., & Loo, S. K. (2018). Sustained effects of neurofeedback in ADHD: A systematic review and meta-analysis. European Child & Adolescent Psychiatry. doi:https://doi.org/10.1007/s00787-018-1121-4
Vernon, D., Egner, T., Cooper, N., Compton, T., Neilands, C., Sheri, A., & Gruzelier, J. (2003). The effect of training distinct neurofeedback protocols on aspects of cognitive performance. International Journal of Psychophysiology, 47(1), 75–85.
Zhang YJ, Duan L, Zhang H, Biswal BB, Lu CM, et al. (2012) Determination of Dominant Frequency of Resting-State Brain Interaction within One Functional System. PLOS ONE 7(12): e51584. https://doi.org/10.1371/journal.pone.0051584
Make a one-time donation
Make a monthly donation
Make a yearly donation
Choose an amount
Or enter a custom amount
I hope you enjoyed reading this post! 🙂
If you’ve found my content helpful, informative, or thought-provoking, I kindly ask that you consider making a donation to help me continue producing new and exciting content for you to enjoy. Your support means the world to me and will allow me to keep bringing you the latest news and scientific insights in the fields of Cognitive Neuroscience, Neurotechnology, Consumer Behavior and Psychology. Any amount, no matter how small, would be greatly appreciated.
Your contribution is appreciated.
Your contribution is appreciated.
DonateDonate monthlyDonate yearly
1 thought on “Neurofeedback: learning to unlock the brain’s self-regulating ability”